Let’s dive into endometriosis as a source of pelvic pain. If you have not already done so, please read my introduction to pelvic pain blog and my ovarian cyst pain blog as a primer for this one.
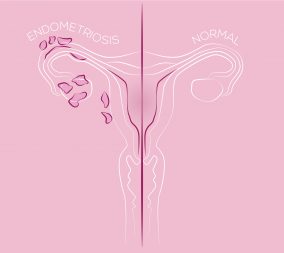
Endometriosis is a relatively common etiology of pelvic pain. It is caused when cells in the lining of the uterus, or endometrium, grow OUTSIDE of the uterus. How do these cells get outside the uterus?!? The most agreed-upon theory is that when a woman menstruates, some of the cells from the uterine lining and menstrual blood exit the uterus backward out of the fallopian tubes. These cells then implant in the pelvis, most often on or near the uterus, tubes, ovaries, and large intestines.
Presentation of symptoms with endometriosis is variable. I was always taught that someone with the most severe endometriosis can be asymptomatic and someone with the tiniest amount can have severe pain. The most common symptom is pelvic pain, especially with periods. However, the pain can be between periods, before/after sex, or with urinating or bowel movements. Some women with endometriosis have a challenging time getting pregnant. (I will not be addressing the effects of endometriosis on fertility in this blog.) Just as I have mentioned in my prior blog posts about pelvic pain, it is not so easy clinically to identify endometriosis. Remember, the brain and body are not wired in a way that tells our bodies the cause of pain. So there are many other conditions that can mimic that pain that is often attributed to endometriosis.
How can we definitively diagnose endometriosis? Some women with endometriosis have a very specific benign ovarian cyst, called an endometrioma, that pretty much confirms endometriosis without having to go to the operating room. However, the only way to know for sure if you have endometriosis is through surgery, where your doctor can visualize the endometriosis, remove as much as is safely possible, and send it to a pathologist for confirmation. It is important to note that if endometriosis is suspected as a possible diagnosis for you, surgery is not always the first line in management. In fact, we often recommend trying medical management first to see if your symptoms improve before introducing the expense/risk of an operation.
Most of the time, treatment of expected endometriosis is with medication. We do this because surgery, while helpful for diagnosis, does not usually provide long-term help with symptoms. In fact, the average symptom-free interval post-operatively is like 6 months. Let’s explore some of the non-surgery options.
- NSAIDs: Non-steroidal anti-inflammatory drugs (alone or in combination with other medications below) can relieve the pain associated with endometriosis for many women. These meds block the release of something called prostaglandins, which are responsible for a lot of pain associated with menstruation. So if NSAIDs are started one to two days before your period, then prostaglandin release can be reduced and thus result in less pain.
- Hormonal birth control: Birth control pills, patches, rings, shots, IUDs (intrauterine devices) can be helpful for the pain because they can be taken in a way to reduce the frequency of or eliminate your period.
- Gonadotropin-releasing Agonists or Antagonists: We do not need to delve into how these meds work specifically; however, they do function to reduce estrogen production from the ovaries and result in decreased pain in up to 80% of patients. Some of the newer medications are antagonists and have the advantage of being taken orally (as opposed to injections). Medicines in this group are often expensive and take time to get insurance prior to authorization.
As mentioned above, surgery can be used for the diagnosis of endometriosis, and for some women at least some short-term treatment/relief. If you are done having children and it is believed that endometriosis is a cause of your pain, then more definitive surgery such as hysterectomy with or without ovarian removal can be on the table as a treatment choice.
I hope this helps as a basic introduction to endometriosis. If you have further questions, please talk to one of our providers about it.